Advancing Surgical Treatments
Revolutionary treatments and innovative care continue to advance the quality of surgical treatments available. The Global Robotics Institute remains at the forefront of these advancements, while delivering an exceptionally comprehensive and supportive patient experience.
New Innovations
- MRI Fusion Biopsy
-
When a Biopsy is Needed
Prostate cancer is notoriously hard to detect. And since the 1980s, screening methods have not changed very much—until recently.
Depending on your age and risk factors, a yearly digital rectal exam is usually performed during your annual well visit. Your doctor will feel for a tumor. However, it only reaches part of the prostate. One downside is it only detects a tumor after it has become large enough to be at an advanced stage.
A PSA (prostate-specific antigen) blood test is also recommended. An elevated PSA level, which may indicate cancer, will prompt a biopsy. In this procedure, tissue samples are taken equally from all zones of the prostatic gland using a thin needle.
However, some men have other conditions that can cause varied PSA readings. In fact, about three-quarters of prostate biopsies come back negative.1 This can be good news for many men, but sometimes it’s simply because conventional methods can easily miss the cancer. As PSA levels continue to rise, a number of biopsies may be needed before the cancer is found.
Imaging the Prostate
For the past 30 years, the conventional method has been to use ultrasound to help guide where to insert biopsy probes. However, ultrasound images are not very clear for this use, and thus cannot detect the suspicious cancer sites. This is especially true for detecting early stages of prostate cancer.
So, this means it is basically a “blind” method where multiple probes are methodically inserted throughout the prostate. The hope is that if cancer is present, at least one of the needles will hit it. But in certain cases the cancer lesions can be easily missed leaving patient without needed treatment.
Limits to Conventional Prostate Biopsy Methods
- Uses ultrasound alone, which does not image prostatic tissue very well.
- There are usually no clear lesions to target. At least 12 core samples are typically taken using a scattershot approach.
- If another procedure is required, cannot accurately map with certainty where the earlier biopsy needle was inserted.
- False negatives, in which treatable (clinically significant) or “active surveillance” (low-risk) cancer is missed, can be as high as 35%.
- Up to half of detected lesions may not be clinically relevant. This can lead to pain and risk for unnecessary treatments.
- Is the only major cancer in which the blind biopsy of an organ is used for diagnosis.
MRI Fusion Biopsy
Today, new medical imaging technology has greatly improved the accuracy of prostate cancer screening.
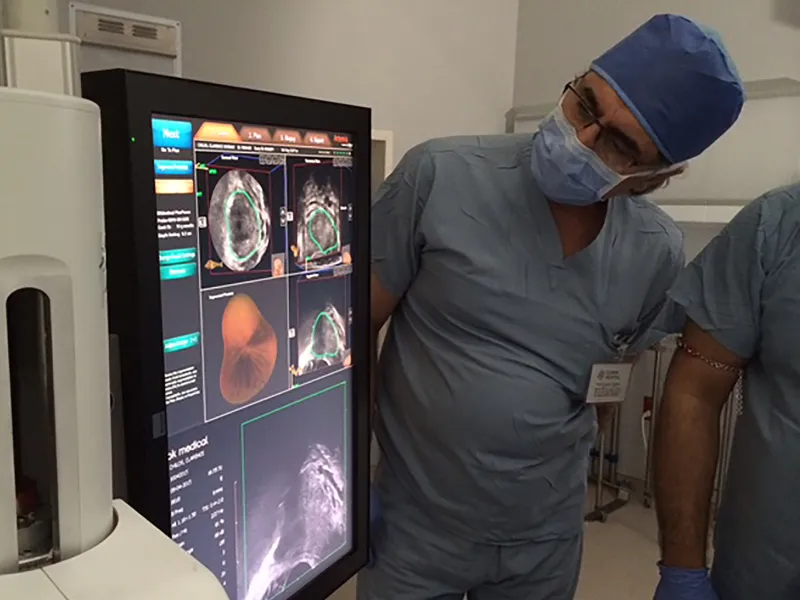
First, a 3T mpMRI (a combination of multiple types and slices of MRI scans) of the prostate is taken and stored. Then, during an outpatient procedure, an ultrasound probe is inserted into the rectum. The two images are fused into a 3D re-creation of the prostate, in real-time. This means that when the probe is moved, the image shifts along with it. The lesion is targeted by the Artemis robot as a suspicious site that needs biopsy. MRI/US fusion robotic guided prostate biopsy is the new standard of care in prostate biopsy care.
Advantages of MRI Fusion Biopsy:
- Combined 3D image has more contrast. This provides a much better image to guide the doctor to specific areas of concern.
- Two- to three-times more (92%) sensitivity for detecting prostate cancer than standard, non-targeted biopsy methods. This means less false-negatives results for aggressive cancers.
- Much less guessing involved. Typically, only a few targeted cores are needed.
- Each biopsy probe is accurately targeted, mapped and tracked. Can return to the same biopsy sites with virtually pinpoint accuracy.
- Can actively track and monitor specific areas of the prostate (for active surveillance) to evaluate if and when treatment is necessary for non-life threatening tumors. Helps reduce over-diagnosis and unnecessary treatments.
Our goal is to provide you optimal care using the best tools available. Due to the many advantages of this screening method, we recommend it for many of our biopsy patients. If you have additional questions about prostate contact us today.
1 Barry MJ. Clinical practice. Prostate-specific-antigen testing for early diagnosis of prostate cancer. New England Journal of Medicine 2001;344(18):1373-1377.
Siddiqui MM, Rais-Bahrami S, Turkbey B, George AK, Rothwax J, Shakir N, Okoro C, Raskolnikov D, Parnes HL, Linehan WM, Merino MJ, Simon RM, Choyke PL, Wood BJ, Pinto PA. Comparison of MR/ultrasound fusion-guided biopsy with ultrasound-guided biopsy for the diagnosis of prostate cancer. JAMA. 2015 Jan 27;313(4):390-7. doi: 10.1001/jama.2014.17942. PMID: 25626035
- High Intensity Focused Ultrasound (HIFU)
-
As a Focal Therapy for Prostate Cancer
The latest advance in prostate cancer treatment is state-of-the-art High Intensity Focused Ultrasound (HIFU). This procedure uses highly concentrated, radiation-free sound waves to ablate (destroy) targeted tissue. Unlike removing cancer tumors from the body surgically, HIFU targets the prostate cancer tumor with ultrasound waves while the prostate stays in place after the procedure.
The heart of the system is a thin, robotic-driven probe used with a transrectal approach. The sophisticated medical device includes both imaging and treatment functions. This permits the surgeon to view ultrasound images of your prostate in real-time during the procedure. The procedure takes one and a half hours to complete and, after the procedure, the patient stays overnight in the hospital (less than 24 hours).
Benefits of HIFU
HIFU was recently approved by the FDA for prostate tissue ablation the United States under protocols of research and study. However, it has been used in other countries for several years with acceptable short-term outcomes. Prior to approval in this country, it was already FDA approved and being used to treat kidney cancer. Men with localized or low grade prostate cancer, or have small tumors are the best candidates for HIFU treatment.
Benefits of the procedure include:
- Minimally invasive procedure carries less risk and produces faster healing
- Ultrasound waves can pass through normal, healthy tissue without damaging it on the way to the targeted tissue.
- Robotic-guided probe precisely targets cancerous areas, resulting in less surrounding tissue being affected, which positively impacts sexual function and early return to continence
- Surgeon views the procedure with ultrasound in real-time, allowing easier adjustments when needed
- You keep your prostate intact and treatment occurs within the target area of the prostate
- No tissue is removed and your body naturally expels the ablated tissue over time
- HIFU treatments can be repeated if cancer reappears for selected cases
- Surgery (prostate removal) and radiotherapy also remain viable treatment options if the cancer returns in the prostate following HIFU
HIFU Treatment
The probe emits HIFU waves that are concentrated into the targeted cancer area of the prostate. Think of it like using a magnifying glass that focuses light waves into a beam. The intensity and scope of the sound energy is adjusted based on the size of the tumor. A robotic-assisted device and surgeon, who views the procedure on-screen as it is occurring, control the movement of probe and guide these functions.
The waves cause the tissue in the ablation area to heat up rapidly, killing the cells within it. A small part of the cancerous tissue is targeted at a time, and then repeated until the entire area is treated. The goal is to kill all cells within the specific target area, which also kills the cancer.
The process is performed under anesthesia and generally takes 2 – 3 hours to complete. Many men can be treated with same-day admission or an overnight stay. High Intensity Focused Ultrasound can be used alone or as part of a wider, comprehensive plan to treat your cancer. And since the prostate is not removed, men must follow a strict regimen to track their PSA levels following the procedure. This will be used to check for any signs of cancer returning.
Electing to Use HIFU
It’s important to note that as an emerging technology, long-term effectiveness and chance of side effects are still being studied. However, its relative strengths are making it a growing treatment option. These include the ability to precisely target cancerous tissue. Plus, data suggests that minimal incontinence and less erectile dysfunction rates occur than in other procedures. It’s important to discuss the gains and potential risks of any procedure with your surgeon before electing to undergo it.
HIFU software enables the operator to target ablation zones with sophisticated planning and localization tools
As with any focal ablative procedure, HIFU carries the risk of reoccurrence and need for retreatment. There is also risk of erectile dysfunction (ED) and urethral stricture.
For information about HIFU treatment at the Global Robotics Institute, click here.
- J-Plasma Bovie
-
J-Plasma is a revolutionary advancement in surgical cutting tools approved by the FDA. Unlike laser, which uses energy in the form of a beam of light to cut, plasma transfers energy through a stream of inert gas (helium). This creates a highly precise surgical instrument. The gas is odorless, colorless and causes no harm to the body.
The use of laser technology in surgical tools was a major advancement when introduced. However, for all its many benefits, lasers also create excess heat energy. The healthy tissue surrounding the incision absorbs this heat, which can damage the cells. Surgeons strive to minimize the spread of this heat during surgeries.
Cold Plasma Transforms Surgery
J-Plasma has solved the excess heat issue found with laser surgical tools. It does this through the innovative use of inert gas to create cold plasma. When electricity is passed through the gas, an energy beam of plasma is created. This beam creates far less heat than laser technology. Plus, the electricity is absorbed back into the device itself and is not transferred through the body.
Benefits of J-Plasma
This highly precise tool can be used for incisions and other cutting tasks. It includes retractable blades for both plasma and traditional scalpel cutting. J-Plasma can also clot blood to minimize bleeding at the surgical site. Plus, it can be set to “paint” tissue at the micron level to kill microscopic layers of diseased surface cells. Read more about the J-Plasma surgical tool here.
Benefits of J-Plasma include:
- Surgeons can achieve an extremely high level of precision and control
- Perfect for use around delicate, vital structures where other surgical tools may cause harm
- Virtually eliminates excess, cell-damaging heat of laser tools
- Plasma technology can kill layers of diseased tissue cell level by cell level, along the surface of body structures
- Because less heat is generated, it can lead to less tissue damage, less pain and quicker healing
- Allows surgeon to cut, coagulate, dissect and use electricity to destroy diseased tissue with single surgical instrument
- Its electric current is non-conductive, so it’s not directed into the body, but into the probe itself
- Multi-functional tool helps surgeon be more efficient, which can shorten surgery times and lessen risks for patients
- Genomic Testing
-
Major advances in genomic testing are developing at a rapid pace. As the cost-benefit curve continues to improve, many new tests are making their way to the average health-care consumer. Utilizing prostate cancer tissue from individual patients, we can now readily identify how aggressively the disease is likely to progress. This gives us the information to truly individualize the course of treatment. Due to the potential positive impact these tests can have on patient outcomes, we have added the following tests to our diagnostic toolbox:
- Decipher ®
- Oncotype ®
- Prolaris ®
- 4Kscore ®
- ConfirmMDx ®
- PCA3 Test
